
Fancy Schmancy
It’s important for practicing clinicians treating voice problems to have a good understanding of how efficiently our patients are using air to vibrate our vocal cords. Coordination is usually impaired when a person has dysphonia of some kind. Dysphonia means hoarseness, or irregularity of the sound signal in some way. We can describe this as breathy, strained, rough, etc.
Pneumotachographs are currently being used in many voice centers to find an aerodynamic measure of transglottal airflow, or TAF. We value this information because it helps us better identify what’s causing a person to be hoarse, and therefore get a treatment plan in action to help.
The Price is Right?
The price for any regular clinician to get a hold of a pneumotachograph would be akin to purchasing a small car. Then after you get one, you are required to keep the maintenance on it, as well as replace it if it breaks. And, frankly, ain’t nobody got money for that. All is not lost. Ashwini Joshi and Chris Watts examined the possibility of using a handheld spirometer (available on many websites) to measure airflow to get a measure of vital capacity. And you know what? They found some pretty applicable information…
What Does It Matter?
They compared a spirometer that costs a person less than $300, and the Phonatory Aerodynamic System from KayPentax. They then found Phonation Quotient (dividing vital capacity by maximum phonation time, found to be clinically applicable by Rau and Becket in 1984). Life-changing and clinic-changing findings are that there were no differences between measurement by pneumotachograph versus the spirometer.
This is incredible news to most every speech-language pathologist in the world because it means that they can use a low-cost handheld spirometer, a maximum phonation time for their patient, and a formula to find a measure of aerodynamics that can be used to plan treatment, as well as measure improvements in current presentations in their patients.
What Do I Use in My Clinic?
I have been using Phonation Quotient to gather aerodynamic measures on my patients since Chris introduced the concept to me in 2014 and encouraged me to read the 1984 article by Ray and Beckett in. I use a Contec Sp10 handheld spirometer with mouthpieces for each patient. (Shown here in the pictures)
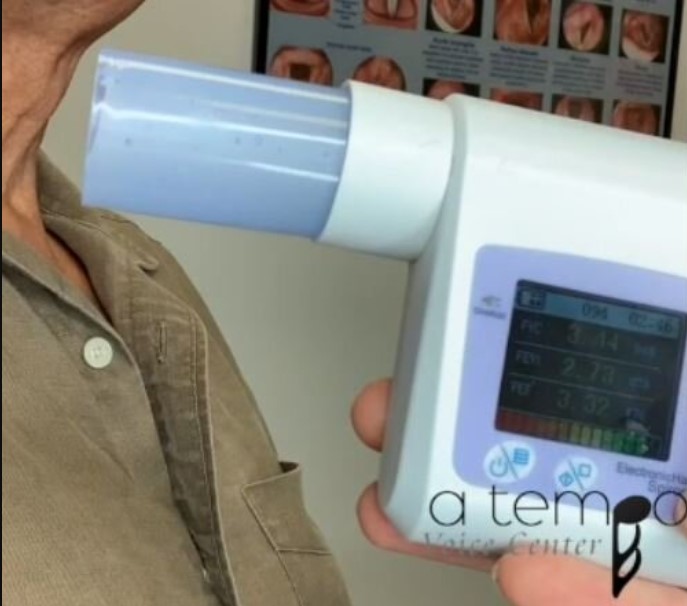


 Moving Forward
Moving ForwardReferences:
Kristie Knickerbocker, MS, CCC-SLP, is a speech-language pathologist and singing voice specialist in Fort Worth, Texas. She rehabilitates voice and swallowing at her private practice, a tempo Voice Center, and lectures on voice science nationally. She is part of the Professional Development Committee for ASHA Special Interest Group 3, Voice and Upper Airway Disorders, and a member of the National Association of Teachers of Singing and the Pan-American Vocology Association. Knickerbocker blogs on her website at www.atempovoicecenter.com. She has developed a line of kid and adult-friendly therapy materials specifically for voice on TPT or her website. Follow her on Pinterest, on Twitter and Instagram or like her on Facebook.


