
As a graduate student in Speech-Language Pathology, there are so many names to learn about with regard to terms coined, rehabilitation techniques researched and therapy approaches we don’t even use anymore. As a patient, you just want answers. Terminology is important, and Christina Kang, Joseph Hentz, and Dr. David Lott have pioneered a term to describe symptoms for dysphagia that does not show up routine swallow studies.
Kang and team took a retrospective look at folks who came into their clinic for swallow and laryngeal studies including VFSS and flexible laryngoscopy. VFSS stands for Videofluroscopic Swallow Study, or Modified Barium Swallow Study, which looks at the swallow function under x-ray with the patient drinking and eating barium. The important thing here is that no swallow weakness or organic pathology was observed in these tests. This means there was no structural cause for the patient complaints. 97% of the patients chosen for this study that were complaining of swallow issues, also had abnormal laryngeal muscle tension. 82 percent had laryngeal hyperresponsiveness. This means that the larynx would respond to stimuli even when it wasn’t present, like in refractory chronic cough, paradoxical vocal fold motion and globus sensation. Inflammation, or swelling and irritation, was also found in 52% of these people.
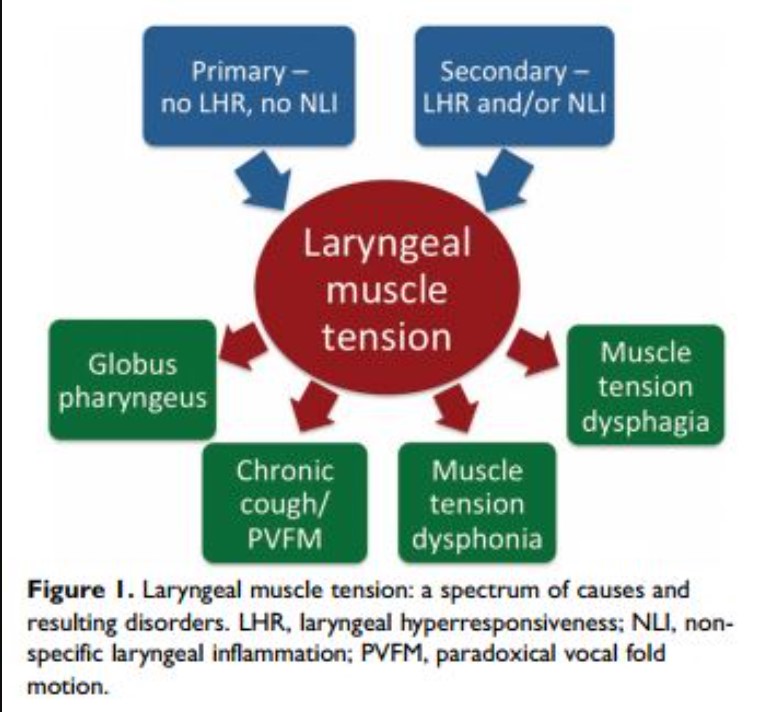
Credit: Kang et al 2016 article.
Kang thought, what if we targeted muscle tension in the larynx through voice rehabilitation, to see if these symptoms resolved? So, 13 of the initial 67 attended voice therapy sessions that specifically focused on unloading muscle tension. Treatments consisted of a combination of Resonant Voice Therapy, Semi-occluded vocal tract exercises, diaphragmatic/low breathing and cirumlaryngeal massage.
Guess What? ALL 13 reported a complete resolution of dysphagia symptoms! Why is this so exciting? I don’t know about you, but these patients seem to get pushed to the side if VFSS shows nothing abnormal, but the patient still feels symptoms. The most common symptom sometimes during my week at the clinic is, “I feel like something is stuck in my throat.” Having complaints seemingly dismissed after a diagnostic test that shows no problems can make the patient upset, feel like it’s “all in my head” and lead to continued and unnecessary testing and physician visits. Kang and team are proposing Muscle Tension Dysphagia or “MTDg” to describe a certain group of patients with functional dysphagia.
The important and amazing thing here is that these patients improved! There is a possible solution to the problems that brought them to the doctor in the first place. We no longer have to send these patients away with no option for treatment.
Of course further testing is needed in this area, but what a great treatment option to offer patients who normally just get sent home and told to “stop worrying about choking, you’ll be fine.”
Reference: Kang, C.H.; Hentz, J.G.; Lott, D.G. Muscle Tension Dysphagia: Symptomology and Theoretical Framework. June 28, 2016.
Kristie Knickerbocker, MS, CCC-SLP, is a speech-language pathologist and singing voice specialist in Fort Worth, Texas. She rehabilitates voice and swallowing at her private practice, a tempo Voice Center, and lectures on vocal health to area choirs and students. She also owns and runs a mobile videostroboscopy and FEES company, Voice Diagnostix. She is an affiliate of ASHA Special Interest Group 3, Voice and Voice Disorders, and a member of the National Association of Teachers of Singing and the Pan-American Vocology Association. Knickerbocker blogs on her website at www.atempovoicecenter.com. She has developed a line of kid and adult-friendly therapy materials specifically for voice on TPT or her website. Follow her on Pinterest, on Twitter and Instagram or like her on Facebook.


